Minimally Invasive Pituitary Tumors
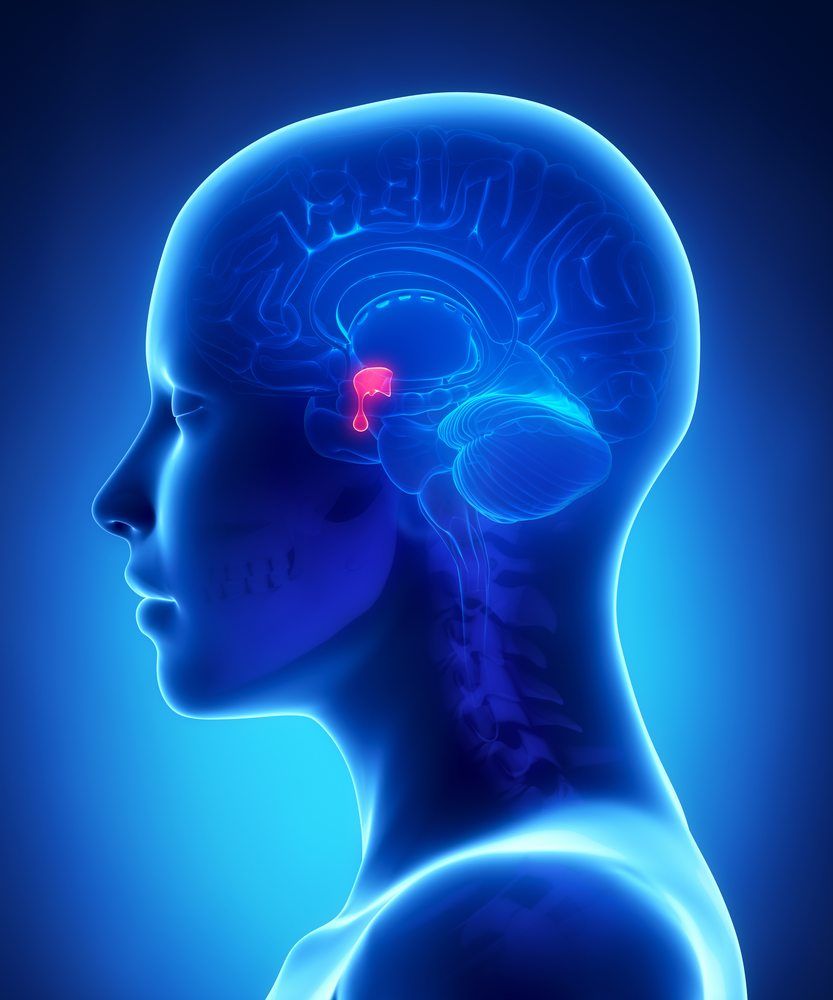
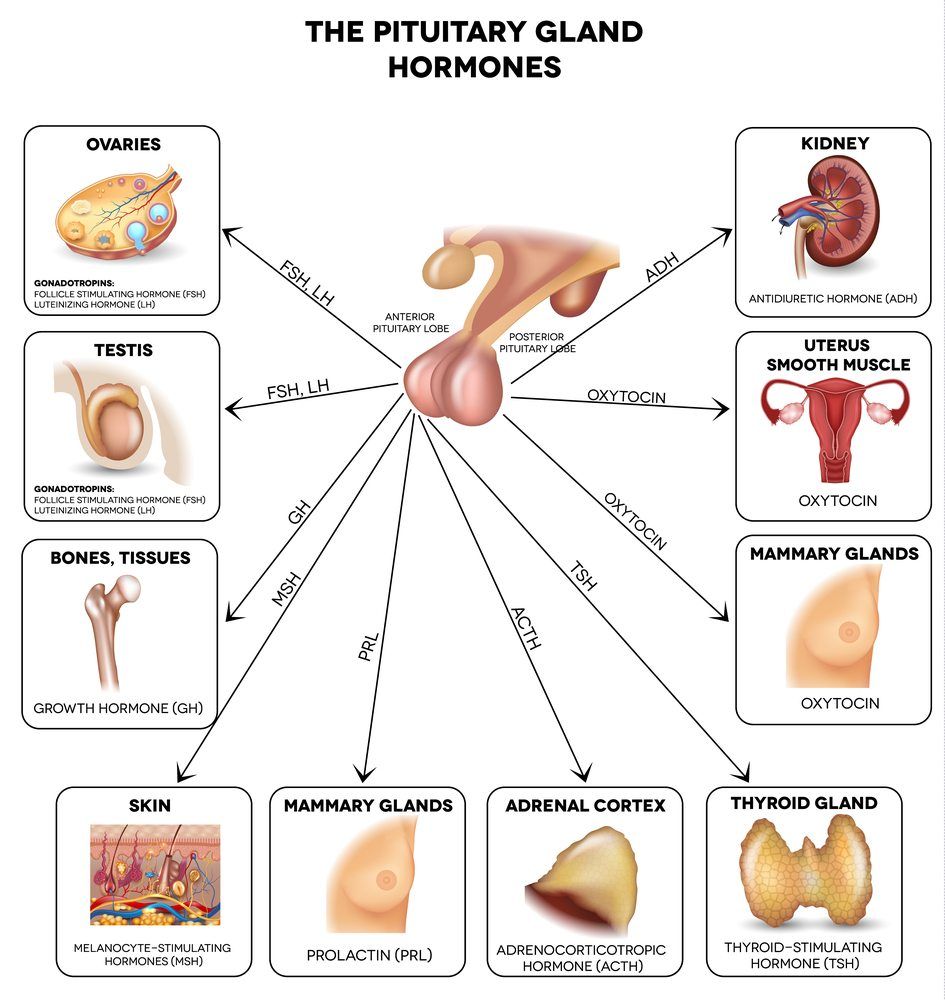
The pituitary gland is situated on the undersurface of the brain toward the center of the head. The pituitary gland is often times referred to as the master gland of the body as it controls many hormonal functions for growth, gender development and serving a very important role in metabolic functions.
Tumors of the pituitary gland are typically benign and are referred to as adenomas.
Adenomas are more common than one might believe and their prevalence in the general population is estimated at 20%.1 Often these pituitary adenomas are asymptomatic and silent. Some are incidentally discover because of a CT scan or MRI of the head was ordered for another reason. Pituitary adenomas are commonly categorized as being large (macroadenoma > 1 cm) or small (microadenoma < 1 cm size) as well as “secreting” or “non-secreting” based upon detection of elevated pituitary hormones in your blood stream.3 About 15-25% of these tumors are more aggressive in their growth rate or invasiveness.4,5
Depending upon their size, growth rate, their ability to secrete hormones and their location, pituitary adenomas can cause symptoms of headache, blindness, double vision, fainting, nausea and vomiting as well as the symptoms associated with hormone imbalances. Hormone secreting tumors can come in many different types that include prolactin-producing (associated with reproductive problems and abnormal breast milk production), adrenocorticotrophic hormone-producing (associated with changes in body fat distribution, osteoporosis, hair growth), growth hormone-producing (associated with enlargement of hands, feet and jaw) and thyrotropin-producing (associated with palpitations and sweating) tumors.
Some pituitary adenomas can cause a life threatening problems related to hormone secretion. A common presentation is vision threatening problems related to pressure on the optic nerves by the tumor. One particularly rare complication occurs when the tumors suddenly bleeds or strangulates itself leading to a condition called “pituitary apoplexy” where severe headach and change in mental status can occur.7 This is a potentially fatal medical emergency which must be treated without delay by surgical decompression in order to have a good prognosis.
Managing pituitary tumors typically requires the involvement of several different physician specialists that function as a “multidisciplinary team”. This multidisciplinary team often includes: a neurosurgeon, an endocrinologist to monitor your hormone levels and an ophthalmologist to follow changes in your vision.
Treatment Options For Pituitary Tumors:
Pituitary tumor treatment options include ongoing observation, drug therapy, surgery, and/or radiation therapy.
1. Observation of silent adenomas is typically offered when tumors are small (microadenoma), asymptomatic without detectable impact on vision, and are non-secreting.
2. Medication (drug therapy) can be effective for treating some secreting (hormone-producing) pituitary tumors. Adenomas that secrete prolactin, called prolactinomas, are treated with Cabergoline which can decrease prolactin secretion and often shrink the tumor. Similarly, adenomas that produce excess growth hormone as well as those that produce excess thyroid hormone can occasionally be treated successfully with Somatostatin analogs like Octreotide®. Ketoconazole (Nizoral®) is used occasionally for pituitary tumors that cause a round face, hump between the shoulders or other symptoms that the body is producing too much of it own cortisol.8
3. Radiation therapy can be recommended: 1. if surgery is not a safe option (eg. recent heart attack) 2. if a pituitary tumor remains or comes back after surgery, or 3. if the tumor causes symptoms that aren’t relieved by medicines. In many cases of radiation, normal pituitary function will be lost and require life-long hormone replacement treatment. Radiation can damage some nearby neural tissue which could affect some function years later, including the optic nerves. Damage here can cause impaired vision or blindness. Lastly although rare, radiation may increase the risk of developing a brain tumor later in life.9
4. Surgery is the mainstay of treatment for most symptomatic or enlarging tumors. The surgery is typically performed with minimally invasive techniques through the nose and is well tolerated with very low risk of serious adverse side effects. The choice for the type of surgical approach is based upon several things including, the position and size of your tumor, surgeon’s preference, and the shape of your nasal cavity. We recommend the approach which is most likely to give your surgeons ample exposure for the safe removal of your tumor.
Surgical Approaches
There are several different surgical approaches to the pituitary gland and most of them involve an approach through the sphenoid sinus. The traditional surgical techniques include a sublabial, (an incision underneath the lip), and trans-septal (an incision inside your nose along your septum) approach. Both of these approaches use the assistance of a microscope for visualization of the tumor and nearby structures. A newer minimally invasive technique is the endoscopic trans-sphenoidal approach. We are mindful of the fact that this minimally invasive approach will shorten your recovery time and it is for this reason that your neurosurgeon has chosen to involve a rhinologist in you care.
What are the advantages of Minimally Invasive Pituitary Tumor Removal (MIPS)?
-
- Faster recovery and less days in the hospital
- Better visualization for more complete tumor removal
- Less intra-operative and post-operative bleeding
- Less complications
- Normalization of nasal function and better preservation of olfaction
- Overall better patient experience
- Four eyes, four hands and two surgeons completely immerse in your surgical procedure!
Why is an endoscope better then a microscope?
An operating microscope offers a straight view of the surgical site and limits the visualization of the lateral aspect of a tumor. Endoscopes have the advantage of the permitting visualization of the tumor in a variety of angles and it can also be used in smaller passageways than an operating microscope alone. This makes the surgery less disruptive to your tissues and provides the least likelihood of affecting your nasal function. In addition, different angles of visualization allows for a more complete and safer tumor resection.










